What is CLN2 Disease?
CLN2 is a genetic disease
CLN2 disease is a rare genetic disorder that affects children.1,2 CLN2 disease is:
- Named after the CLN2/TPP1 gene, which is mutated (abnormal) in CLN2 disease2
- One of the most common forms of neuronal ceroid lipofuscinosis (NCL)2
- NCLs are a group of inherited disorders, which are collectively known as Batten disease3
- Previously known as late-infantile NCL because, for most children, symptoms begin between the ages of 2 and 42
CLN2 disease is an inherited disease that is passed down through families
Children with CLN2 disease are born with this condition, even though it may take months or years before they start showing signs.2
CLN2 disease is referred to as an autosomal recessive disorder2
- Everyone has two copies of the CLN2 gene. In people with CLN2 disease, both inherited genes (one from each parent) have mutations2
- Parents of a child with CLN2 disease have a mutation in one of their CLN2 genes2
- Parents are carriers of the genetic mutation, which means they are healthy but can pass on the mutation to their children2
- If both parents carry the mutation and have a child, there is a2
- A 25% chance that the child will inherit both mutations and be affected by CLN2 disease and experience symptoms
- A 50% chance that the child will be healthy, but they will also carry the one mutation for CLN2 disease
- A 25% chance that the child will not carry any mutation for CLN2 disease and will not have CLN2 disease
How is CLN2 diagnosed?
Diagnosis can be confirmed through genetic testing, which looks for a mutation in a DNA sample collected from the child. CLN2 diagnosis can also be confirmed through enzyme testing, which looks for low levels of the TPP1 enzyme.4
CLN2 disease is a type of lysosomal storage disorder that affects cells in the brain5
There are lysosomes inside every cell. Lysosomes contain enzymes that break down and recycle material in the cell. One of these enzymes is called TPP1.5
The TPP1 enzyme is missing or does not work properly in children with CLN2 disease. When this enzyme isn't working correctly, certain materials build up in the lysosomes of cells, particularly cells in the brain and the eyes.3,6
CLN2 disease is associated with a build-up of materials inside brain cells3,6
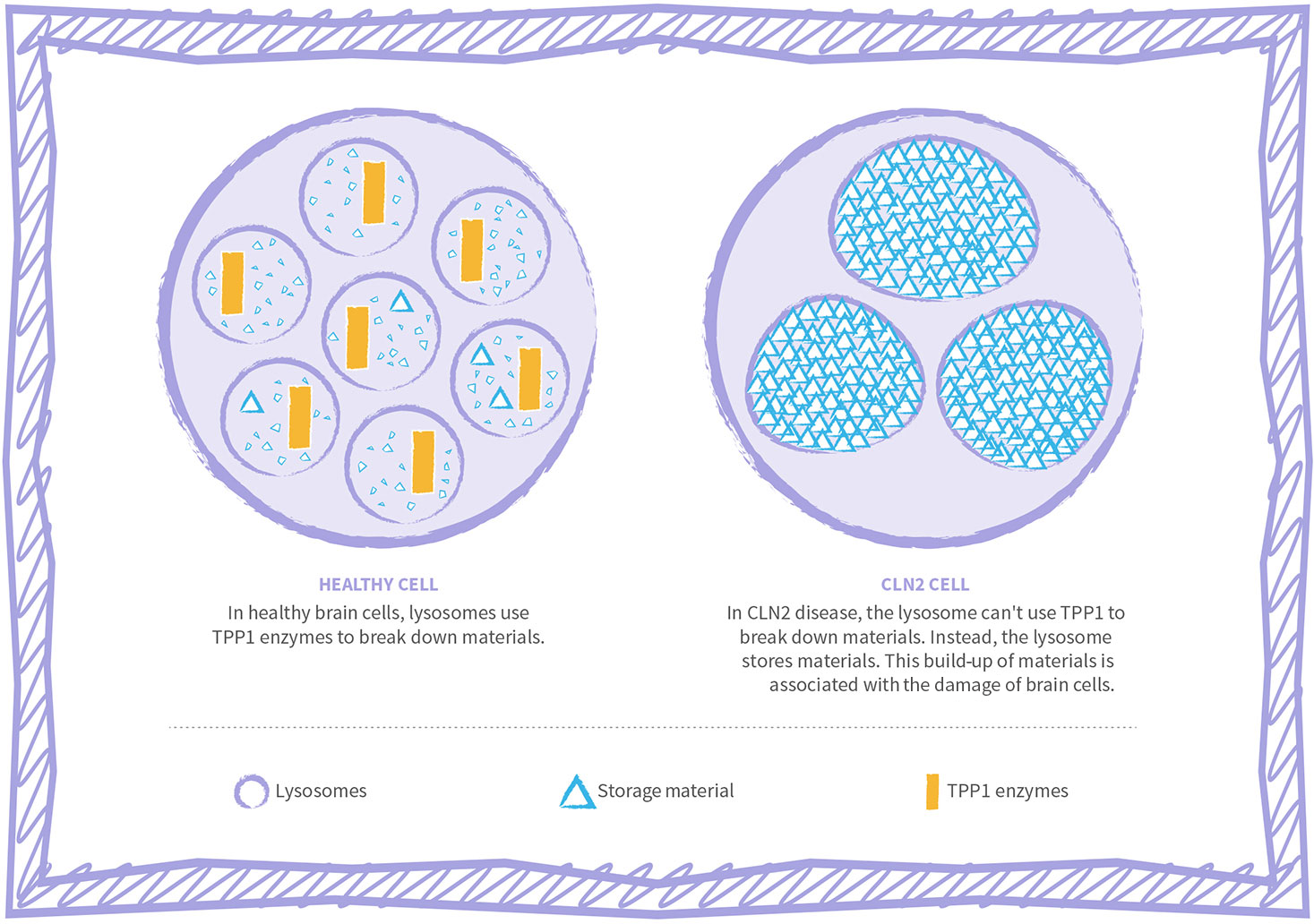
Over time, this build-up is associated with damaging the cells in the brain and the eyes, and they stop functioning normally. As this happens, the symptoms of CLN2 disease (for example, language development delay, seizures and visual impairment) appear.1,3
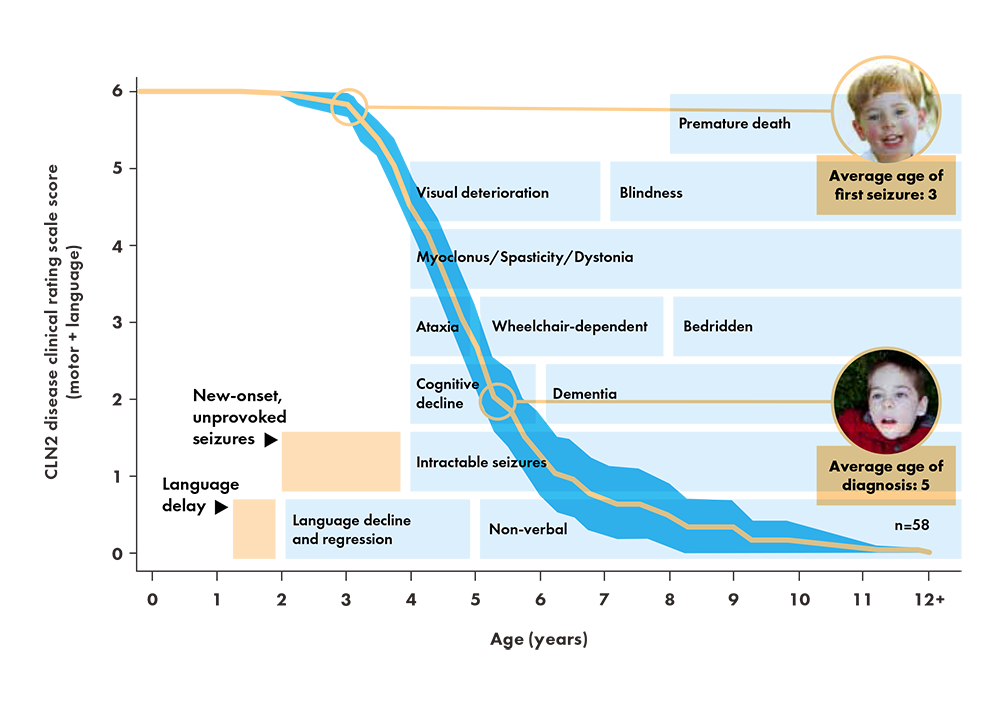
When do the symptoms of CLN2 disease usually appear?
The symptoms of CLN2 disease usually get worse over time and include the following:2,5,7-11

- Kohlschütter A, Schulz A. CLN2 disease (classic late infantile neuronal ceroid lipofuscinosis). Pediatr Endocrinol Rev. 2016;13(Suppl 1):682-688.
- Mole SE, Williams RE. Neuronal ceroid-lipofuscinoses. 2001 Oct 10 [Updated 2013 Aug 1]. In: Pagon RA, et al., eds. GeneReviews®.
- Haltia M. The neuronal ceroid-lipofuscinoses: from past to present. Biochim Biophys Acta. 2006;1762:850-856.
- Fietz M et al. Diagnosis of neuronal ceroid lipofuscinosis type 2 (CLN2 disease): Expert recommendations for early detection and laboratory diagnosis. Mol Genet Metab. 2016;119:160-167.
- Mole SE et al. Correlations between genotype, ultrastructural morphology and clinical phenotype in the neuronal ceroid lipofuscinoses. Neurogenetics. 2005;6:107-126.
- Schulz A et al. NCL diseases–clinical perspectives. Biochim Biophys Acta. 2013;1832:1801-1806.
- Chang M et al. CLN2. In: Mole S, Williams R, and Goebel H, eds. The neuronal ceroid lipofuscinoses (Batten Disease). 2nd ed. Oxford, United Kingdom: Oxford University Press; 2011:80-109.
- Pérez-Poyato MS et al. Late infantile neuronal ceroid lipofuscinosis: mutations in the CLN2 gene and clinical course in Spanish patients. J Child Neurol. 2013;28:470-478.
- Worgall S et al. Treatment of late infantile neuronal ceroid lipofuscinosis by CNS administration of a serotype 2 adeno-associated virus expressing CLN2 cDNA. Hum Gene Ther. 2008;19:463-474.
- Steinfeld R et al. Late infantile neuronal ceroid lipofuscinosis: quantitative description of the clinical course in patients with CLN2 mutations. Am J Med Genet. 2002;112:347-354.
- Nickel M et al. Disease characteristics and progression in patients with late-infantile neuronal ceroid lipofuscinosis type 2 (CLN2) disease: an observational cohort study. Lancet Child Adolesc Health. 2018;2:582-590.

 Deutsch
Deutsch عربى
عربى Français
Français Hrvatska
Hrvatska Русский
Русский Türkçe
Türkçe Română
Română